 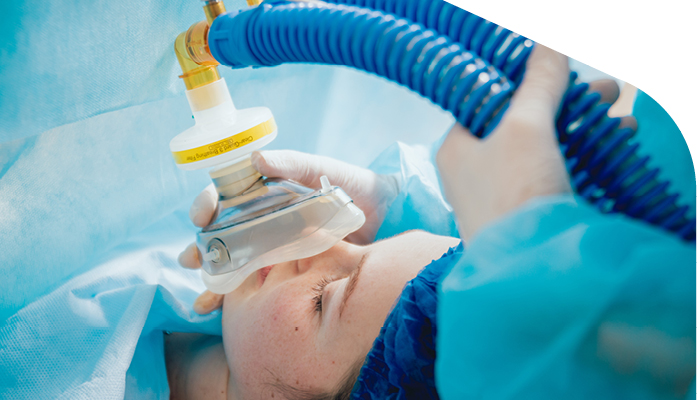
The main properties of these fibres are summarised in the table below. Nociceptors can be divided into two main classes A-delta and C fibres. Nociceptors are probably activated by mechanical distortion of the nerve leading to an increase in H + and K + concentration. Providing the stimulus is suitably intense, high threshold nociceptors will still activate in the absence of actual tissue damage. These are un-encapsulated free nerve endings that are present in the skin, deep somatic tissue and viscera. Addressing the patient’s anxieties can reduce the severity of pain sufferingĪcute pain perception begins with activation of specific sensory nerves, termed nociceptors.Emotion can have a significant impact on pain perception.Attention must therefore be paid to the psychological and emotional state of the patient and address these issues at an early stage with appropriate preparation, explanation and reassurance to ensure optimal pain control. This gives rise to an altered affective state where patients may be irritable, anxious and afraid and this can feedback to further exacerbate the problem. An expectation of pain may in itself lead to an increase in perceived pain and a limited response to analgesics. For example, a patient may have previously experienced severe post-operative pain that can lead to fear and anxiety of subsequent surgery. Pain has strong sensory and emotional components that interact together to produce an overall ‘pain experience’. The majority of patients will fall between these two extremes but demonstrates that good pharmacological management and procedural skills, though essential elements of pain management, can be inadequate if used in isolation. For example, some patients may only gain pain relief from doses of opioids that render them unconscious while others may not require strong opioids at all. It is not uncommon in anaesthetic practice to encounter patients who have very different analgesic requirements despite undergoing identical surgical procedures. The overall perception of acute pain is however not always entirely determined by, or proportionate to, the degree of tissue damage. Rather, there is a complex interaction with other neural processes that may augment or diminish the signal at different stages. However, the steps in conveying the nociceptive signal from the peripheral nerves to the brain should not be regarded as a simple relay system. Once a threshold has been reached, an action potential is produced that travels along a peripheral nerve, through the sensory cell bodies of the dorsal root ganglion and into the spinal cord before ascending to the brain. These nerve endings transduce physical and chemical stimuli in a logarithmic scale depending on the intensity of stimulus applied. Nociceptive signals exert profound changes within the peripheral nervous system in response to injury but also extend to affect the spinal cord, higher centres within the brain and remote organ systems through the neuro-humeral and endocrine response.Īcute pain is detected in the peripheral nervous system by specialised primary nerve fibres known as nociceptors. Physical, thermal or chemical stimuli initiate a cascade of events that lead to predictable physiological, psychological and behavioural responses. In most circumstances, acute pain is self-limiting and proportionate to the degree of injury sustained. 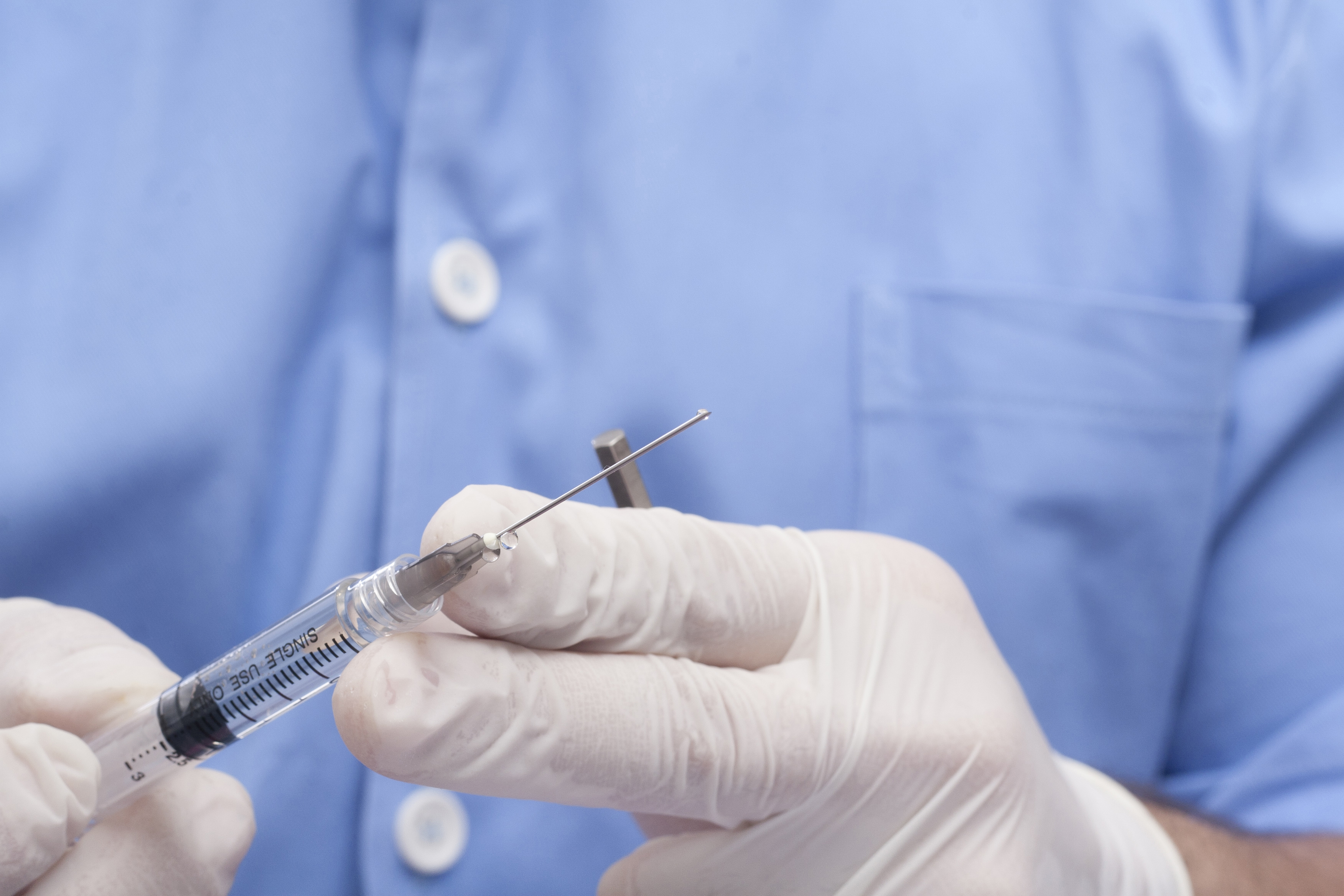
In evolutionary terms, acute pain serves an essential role for the individual as it informs of actual or impending tissue damage. 
It is the hope of the authors that this series will help to equip the reader with the knowledge to improve their ability to recognize and treat pain more effectively. This finding has been repeated throughout the world in different cultures and healthcare settings. Research has consistently demonstrated that pain is very commonly under-recognised and under-treated. They are written for a broad audience and consequently will start from a basic level. This series of tutorials aims to explain current knowledge of the basic science underlying pain mechanisms and treatment, with later tutorials covering the clinical management of specific pain problems. Subsequent research has made significant advances in identifying the mechanisms that underpin acute pain its physiological and clinical consequences and the multifactorial nature of pain perception. This followed publication of the first guidelines and studies of best practice in Australia in 1988. Despite this fact, it is only within the past 20 years that the importance of acute pain has been fully recognised. Can be activated by electrical stimulusĪcute pain is a common reason for presentation to hospital for many medical and surgical pathologies as well as being a key component of successful anaesthetic management.Is influenced by a patients psychological state.Is usually proportionate to the injury sustained. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
